Obstructive Sleep Apnea (OSA) is a sleep disorder where the muscles that support the soft tissues of the throat temporarily relax. When these muscles relax, the airway is narrowed or closed, and breathing is momentarily cut off, causing an apnea. Patients with OSA can have anywhere between five to 100 apneas an hour. OSA affects over 22 million diagnosed Americans alone, though it is estimated that 80% of OSA goes undiagnosed.
The Dangers of OSA:
According to the National Commission on Sleep Disorders Research, approximately 38,000 deaths occur per year due to OSA–related cardiovascular issues. These issues include high blood pressure, hypertension and stroke, among others. In fact, sleep apnea may increase the risk of mortality in those patients who previously suffered a stroke.
In addition to cardiovascular disease, OSA has several other risks including but not limited to: diabetes, metabolic syndrome, dementia, Alzheimer’s disease, daytime sleepiness, and nighttime bet wetting. Treating OSA properly will improve quality of life and decrease other ailments. Treatments range from surgery, to breathing machines, to Oral Appliance Therapy (OAT). Most sleep medicine practitioners direct patients immediately to breathing machines as the industry standard; however, this is not always the best and most beneficial form of therapy in many cases.
Problem: The CPAP works, but is often not used consistently or is not tolerable to patients
Those suffers with moderate-to-severe OSA are systematically guided to the Continuous Positive Airway Pressure (CPAP) machine, which is in-line with American Academy of Sleep Medicine (AASM) guidelines. However, many people do not use the CPAP consistently enough to reach the recommended 7.5 hours per night to be effective. Partial adherence is not enough for efficacy to be reached as patients need to complete at least two of the three sleep cycles for results. Many patients cannot tolerate the CPAP machine for the length of time required for full benefit. It is also recorded that CPAP usage ranges between 30 – 60% in a paper by Terri Weaver and Amy Sawyer. This is not enough consistency to show benefit or prevent cardiac issues.
When the CPAP is used for less than half of the sleep period, it does not reduce frequency of death from heart attack. There are ways to solve this unfortunate issue, and one way is to complement the CPAP with OAT.
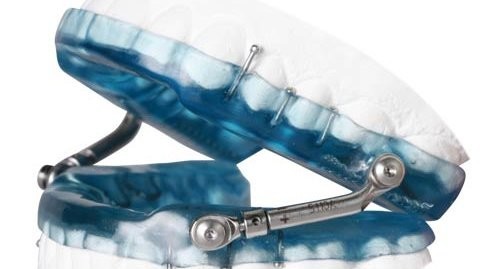
Solution: Add a MAD to CPAP therapy and use it during the part of the night when the CPAP is taken off.
Patients who take the CPAP off during the night can continue their therapy for the evening with a Mandibular Advancement Devise (MAD). MADs have shown to be just as effective as the CPAP in positively impacting cardiac autonomic function during the daytime. MADs are custom made by certified sleep dentists and are an easy, portal, and consistent way to treat sleep apnea, and are generally recommended for mild-to-moderate OSA. For those patients who primarily use the CPAP, a MAD can be critical in reaping maximum therapy benefit when patients are not tolerant of the CPAP in general or can only tolerate limited usage each night. When used together, optimal results can be achieved.